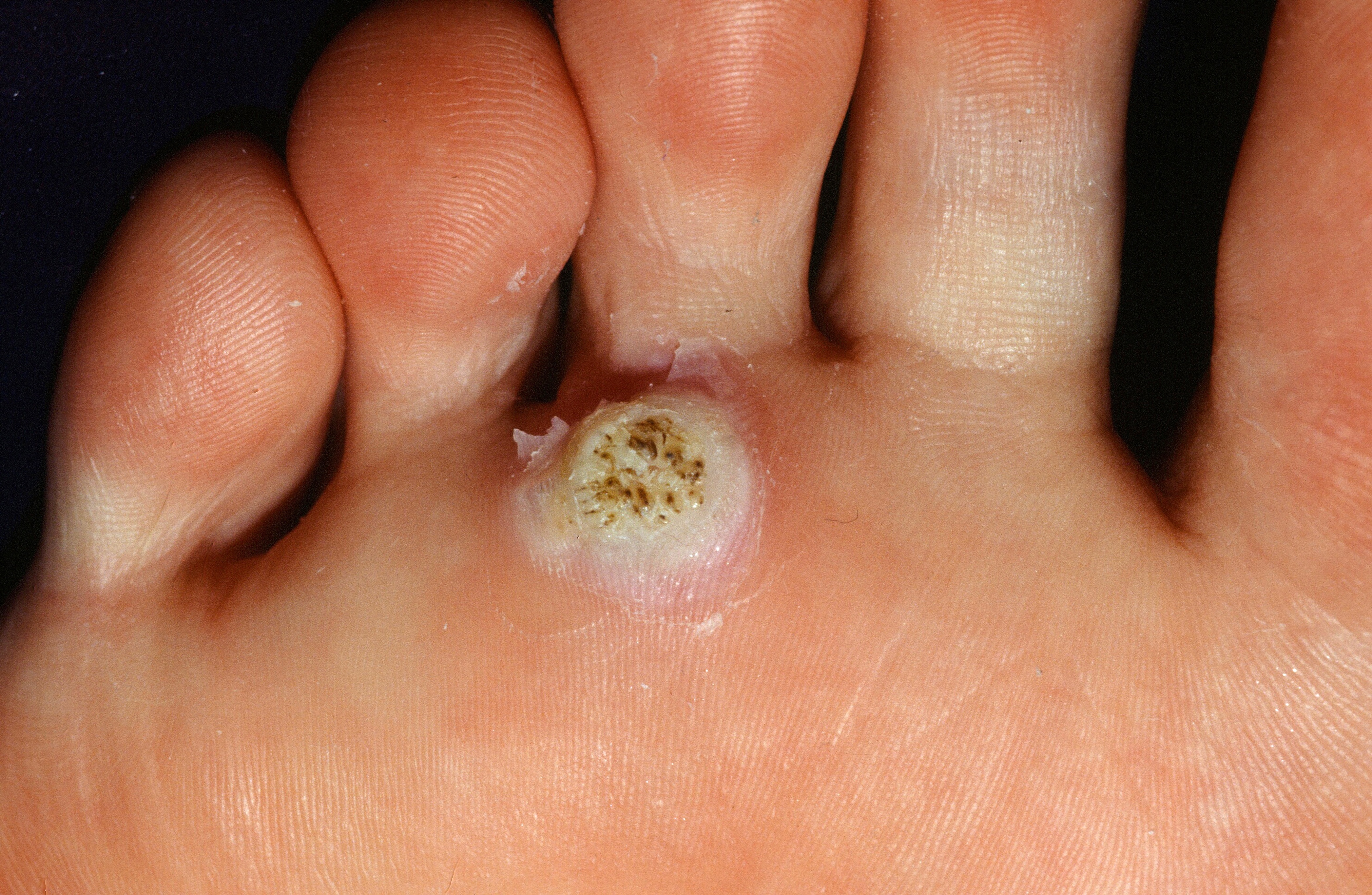
"After freezing a wart, the treated area will become red and irritated and often forms a blister within 24–48 hours—this is expected and means the treatment is working. The blister may dry up and crust over or collapse and peel, and healing usually takes 1–3 weeks, sometimes longer on the hands or feet. If a blister becomes tense or painful, you may carefully pop it with a clean needle and keep the area clean, then apply plain petroleum jelly (Vaseline) until healed. Warts often require 3-5 treatments, so do not be concerned if the wart does not completely resolve after a single freezing."
Warts or verrucae are skin lesions caused by infection by human papillomavirus (HPV).
Warts come in many shapes and sizes. The most common is the hyperkeratotic, verrucous papule on the hands or feet of a child. Flat warts are slightly raised, flat papules or small plaques. Occasionally, they may resemble nevi. Many warts are exophytic (stick out), but lesions on the soles are usually endophytic (extend into the skin) because of the constant pressure. Warts commonly occur about the nails, especially in children who bite or pick their nails. Warts do not show fingerprints, in contrast to calluses.
Darker-skinned patients get warts less commonly which is fortunate given that cryotherapy easily induces white spots after therapy.
If located on the sole, be sure to confirm the diagnosis by paring. A wart has black dots; a corn has a clear center. Verrucous lesions that resist treatment should be biopsied. Occasionally a squamous cell carcinoma or even an amelanotic melanoma may be found. Subungual lesions in an adult should raise particular concern and prompt biopsy sooner rather than later to rule out squamous cell carcinoma).
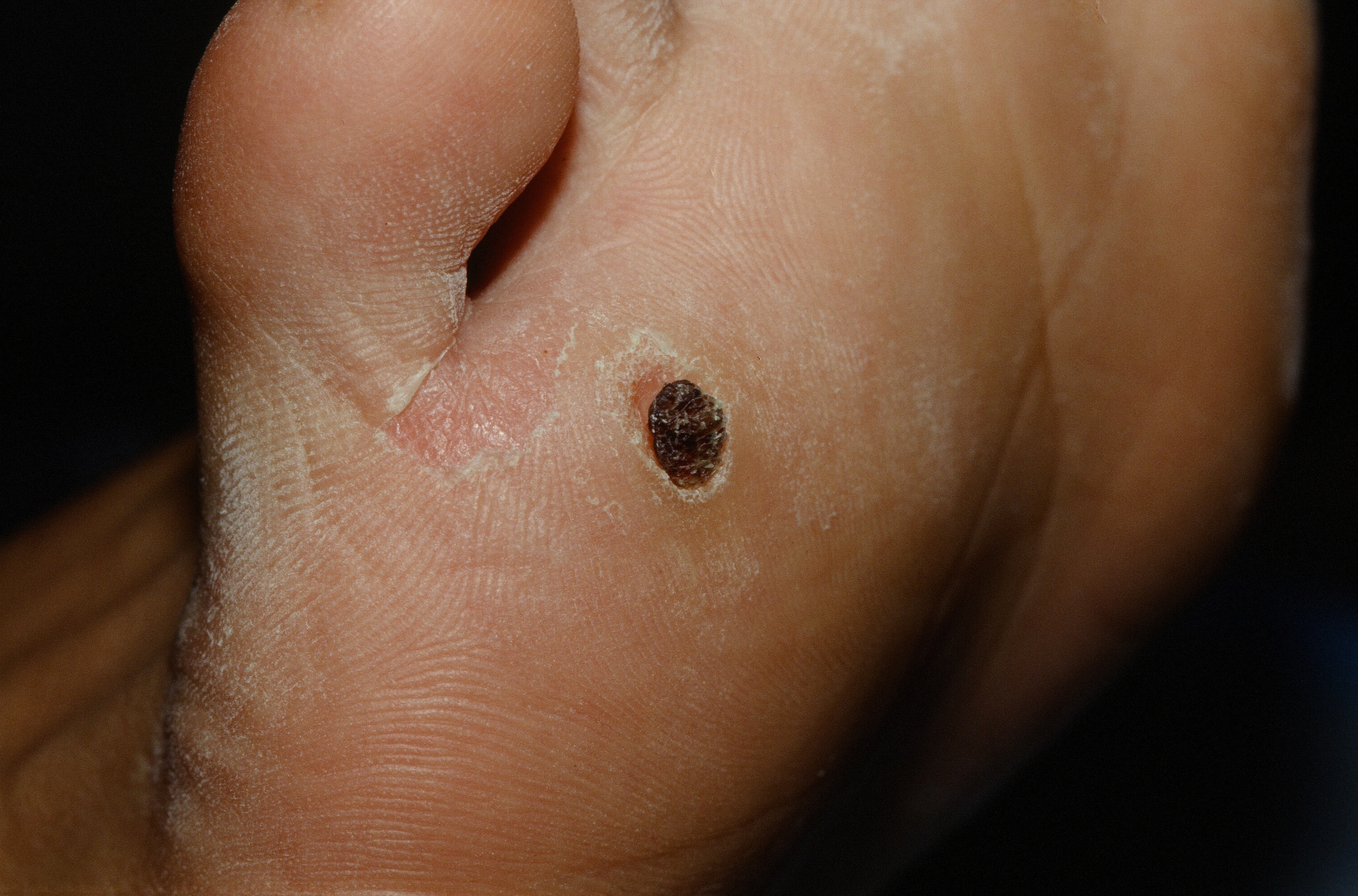
When the immune system finally wins and kills the wart, it dries up, turns brown/black and falls off.
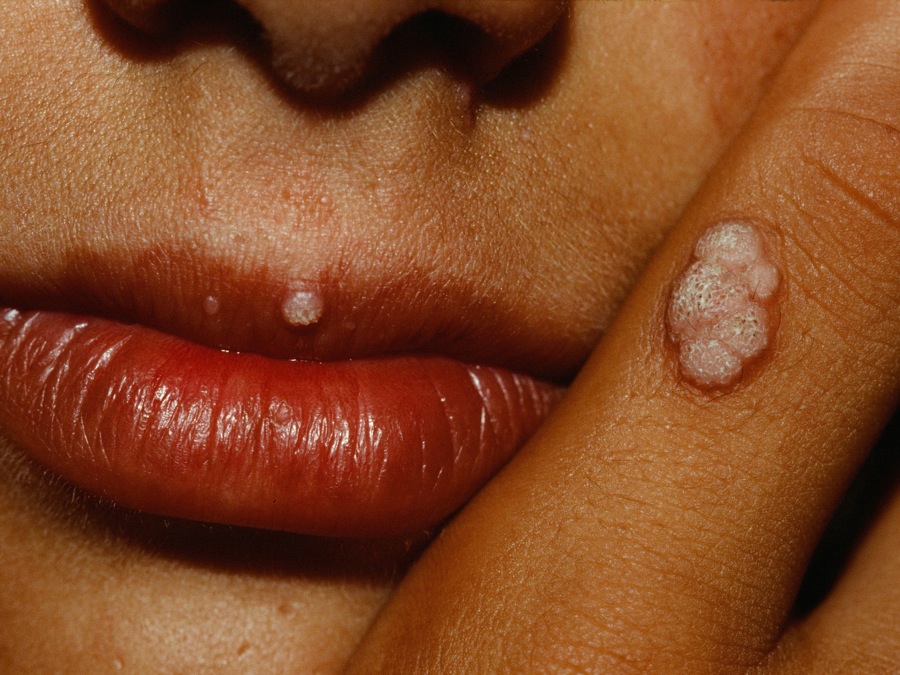
Warts may be spread through autoinnoculation.
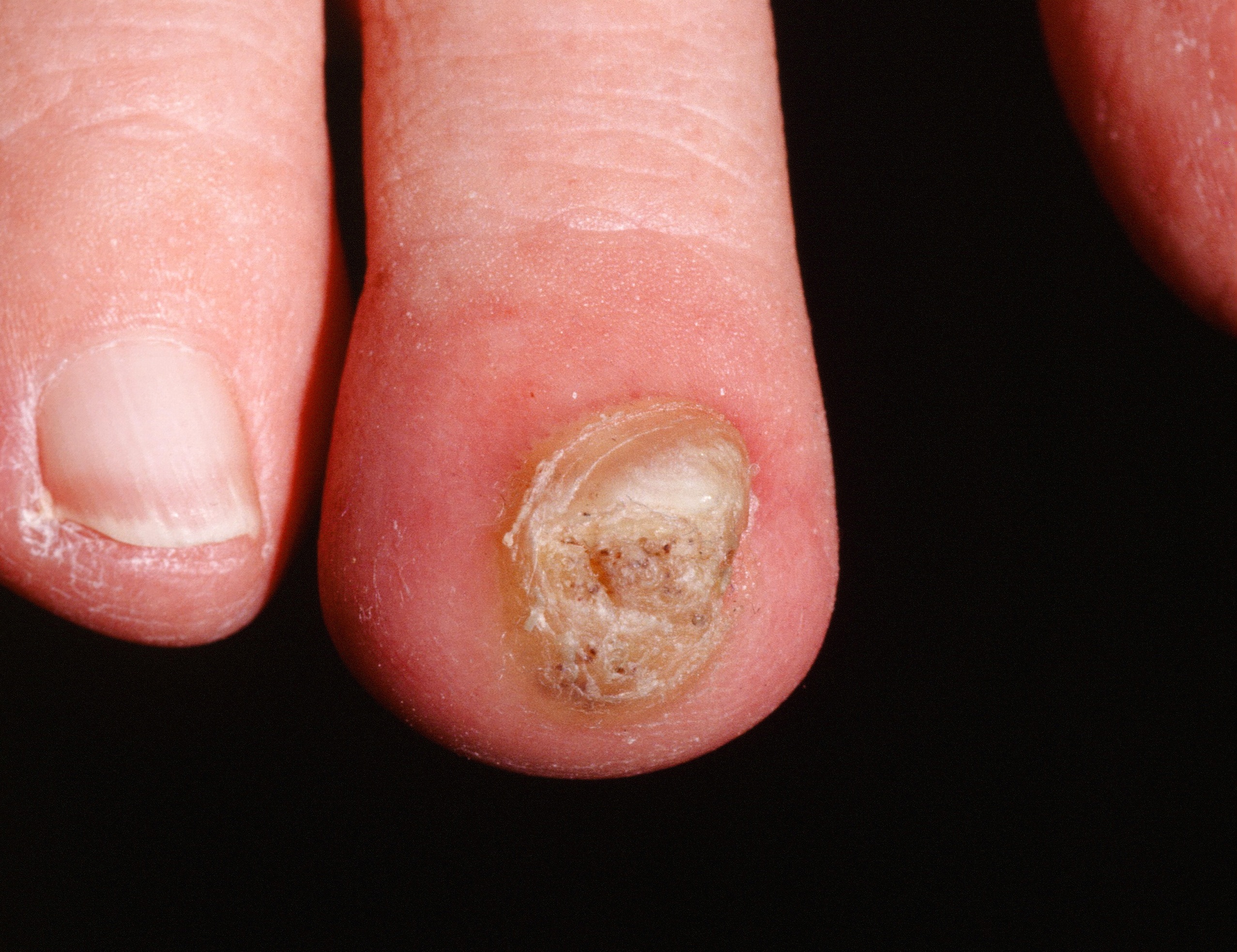
A subungual wart. For longstanding lesions, especially in older patients, a biopsy to rule out squamous cell carcinoma may be in order.
Homepage | Who is Dr. White? | Privacy Policy | FAQs | Use of Images | Contact Dr. White