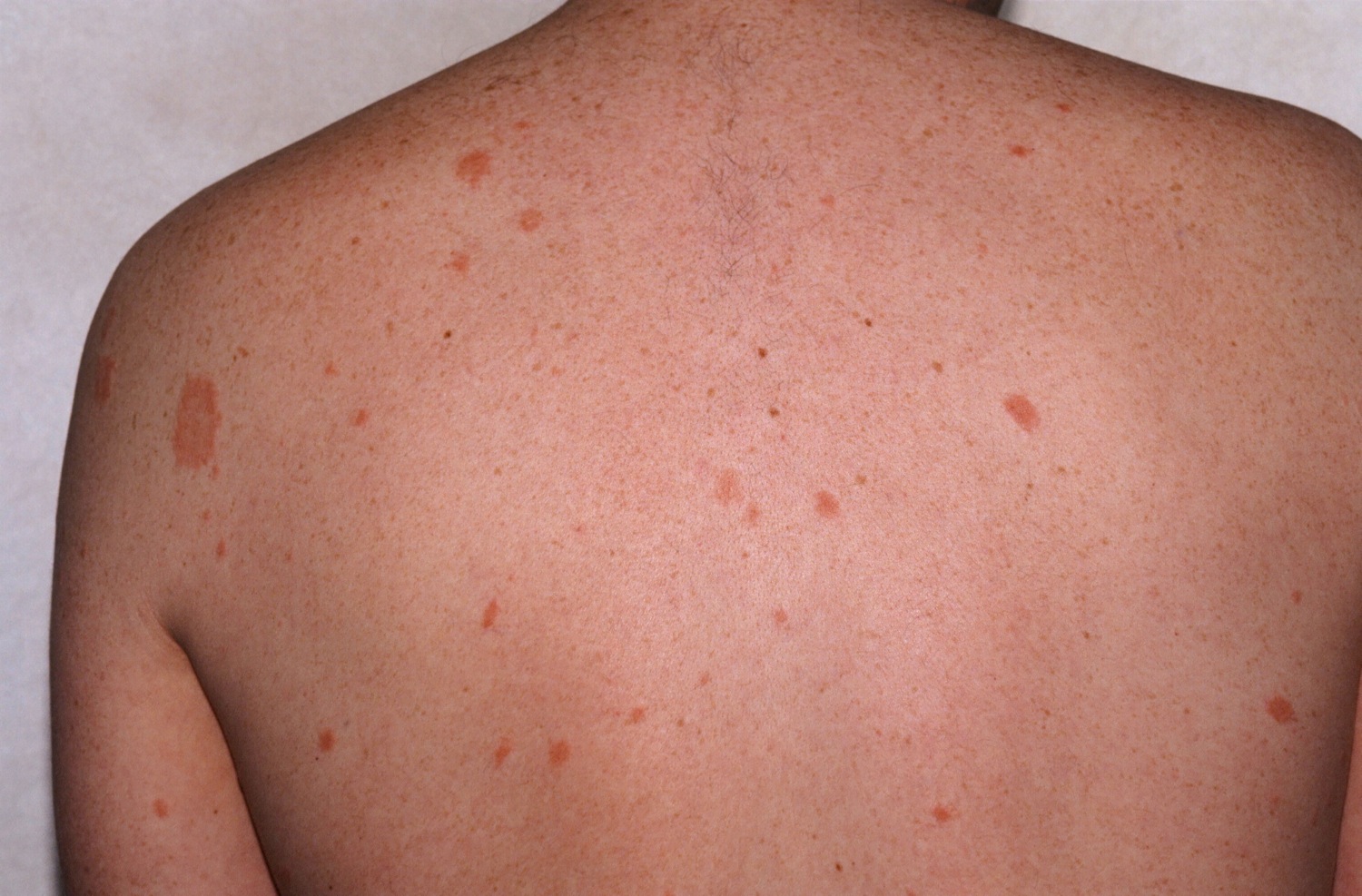
Classic herald patch, the "mother," on the left shoulder, with secondary lesions, the "babies," scattered around on the back.

Classic herald patch, the "mother," on the left shoulder, with secondary lesions, the "babies," scattered around on the back.
Pityriasis rosea (PR) is a common, benign, self-limited papulosquamous skin condition affecting primarily children and young adults. Seventy-five percent of patients are from 10 to 35 years of age.
There is no internal involvement. It is somewhat more common in the winter. Most cases occur in isolation, but occasionally there will be two family members affected. Various drugs have been reported to have caused a PR-like eruption, but it is highly unlikely that a drug can cause the classic presentation of a herald patch followed by secondary lesions.
Probably. Why?
In many patients, a herald patch appears first. The herald patch is round to oval, red and scaly, and may be from 2-6 cm in diameter. It typically occurs on the trunk, neck or proximal extremities. When a patient presents with a solitary papulosquamous lesion of short duration, think PR.
One to several weeks later, the patient experiences a diffuse eruption of red, oval plaques on the trunk, axilla, sides of neck and the groin. PR definitely prefers the sun-protected areas and this is a helpful diagnostic sign. The palms and soles are usually spared (as compared to secondary syphilis where they are usually involved). Many of the plaques may be noted to have a collarette of scale which is also a helpful diagnostic sign. Usually, the long axis of the plaques runs parallel to the ribs giving a Christmas tree pattern.
The areas hidden from the sun like the axilla, buttocks and groin are preferrentially affected. For pictures that are NSFW (not safe for work) see here.
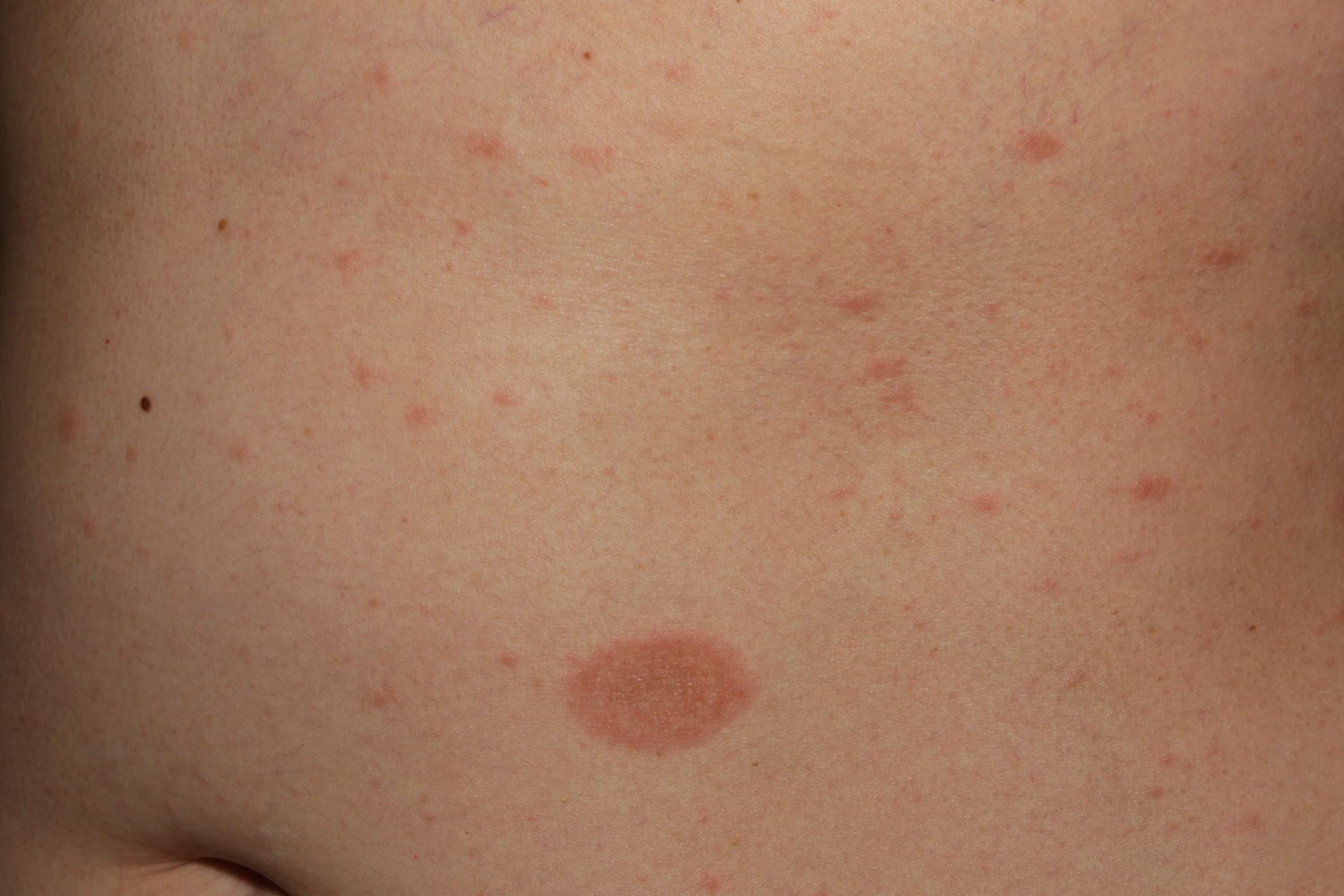
A mother (herald) patch and multiple babies.
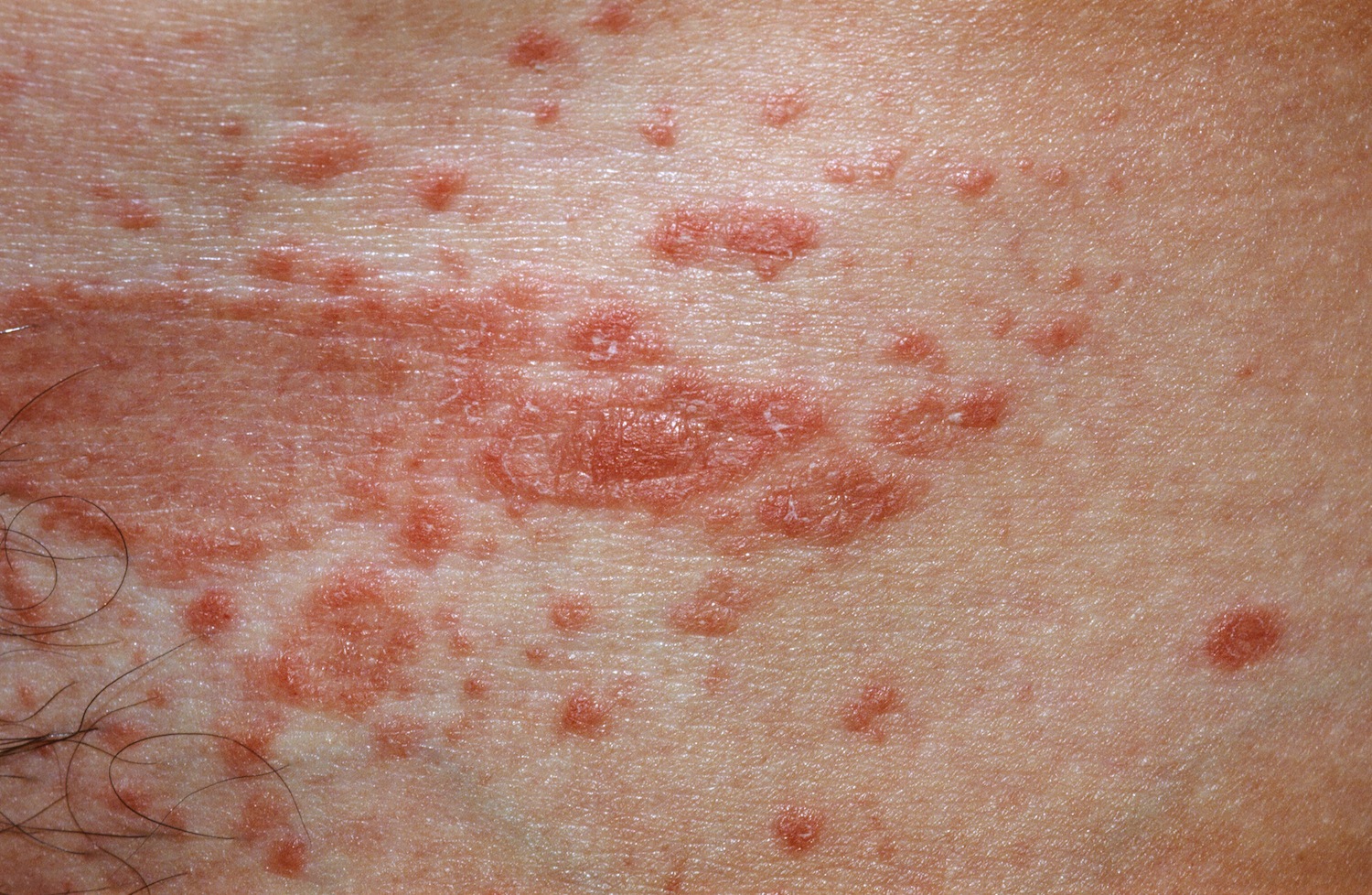
Papules coallescing into plaques in the groin.
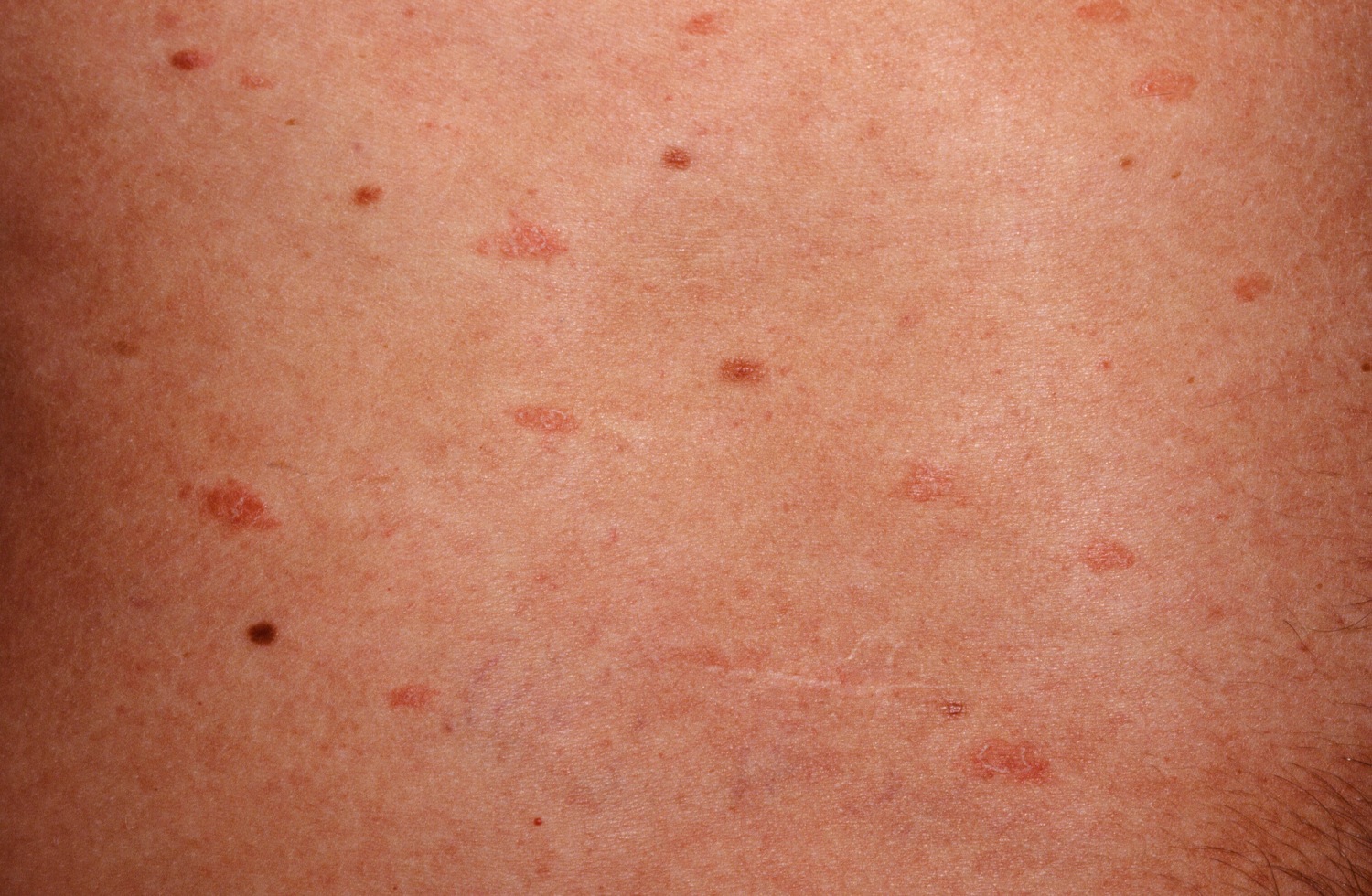
Notice the linear, parallel structure.
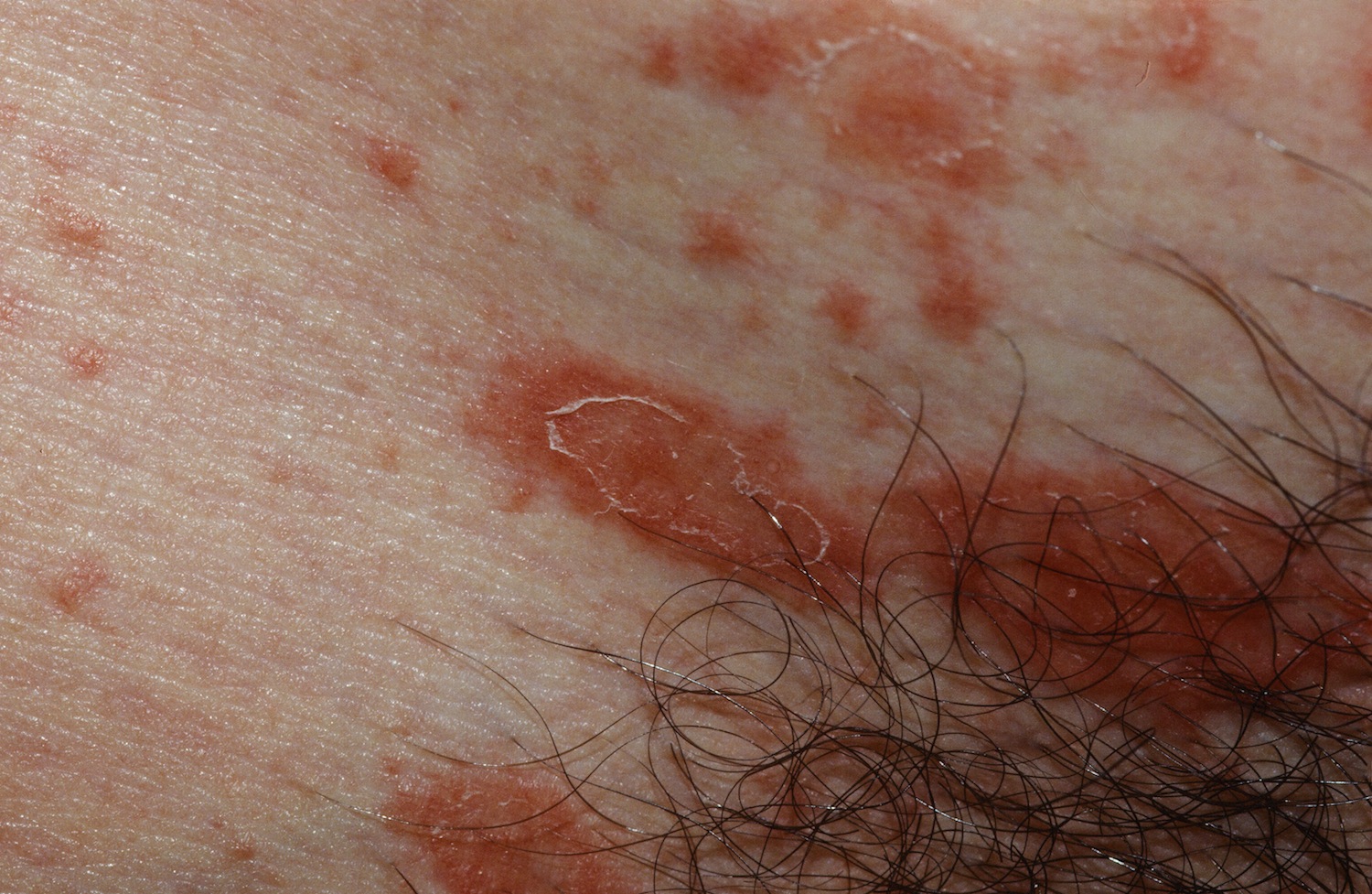 The classic collarette of scale. Notice how the plaque is oriented along the skin lines.
The classic collarette of scale. Notice how the plaque is oriented along the skin lines.
Homepage | Who is Dr. White? | Privacy Policy | FAQs | Use of Images | Contact Dr. White