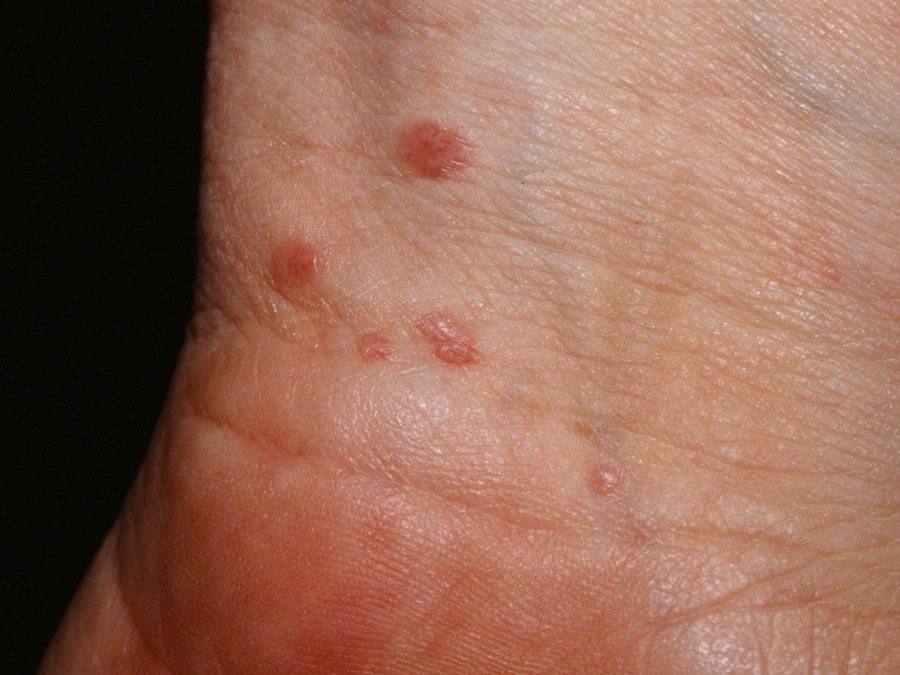
 Purple, pruritic papules on the inner wrist.
Purple, pruritic papules on the inner wrist.
 Purple, pruritic papules on the inner wrist.
Purple, pruritic papules on the inner wrist.
Lichen planus (LP) is a chronic inflammatory condition that can affect the skin, mouth, nails, and genitals, causing itchy, purple, flat-topped papules and plaques, sometimes with lacy white patches in the mouth.
Itchy, violaceous to purple papules and plaques are typical. The surface often has a characteristic white, lacy pattern, called Wickham's stria. As individual lesions heal, residual pigmentation in the form of post inflammatory hyperpigmentation is common. Koebnerization may occur and pruritus may be intense. The inner wrists, ankles, sides of feet, back, oral mucosa, vulva and penis are favored sites. However, the entire body may be covered in severe cases. Thickened, hypertrophic lesions are more common on the legs. A variant of LP in the sun-exposed areas is called lichen planus actinicus. Milia may develop. Rarely bulla may form. The nails may become dystrophic. Very rarely, lesions may occasionally be scaly, putting them in the papulosquamous differential.
An ever-growing number of drugs have been noted to cause lichen planus-like eruptions. These include the new biologics, antimalarials, arsenicals, beta blockers, captopril, furosemide, gold salts, methyl dopa, penicillamine quinidine, sulfonylurea, salsalate and thiazides. One patient's LP was caused by gold-containing cinnamon schnapps. There is some variation in nomenclature. Do these drugs induce lichen planus or do they cause a lichenoid drug eruption? This site has chosen to use the term lichenoid drug eruption.
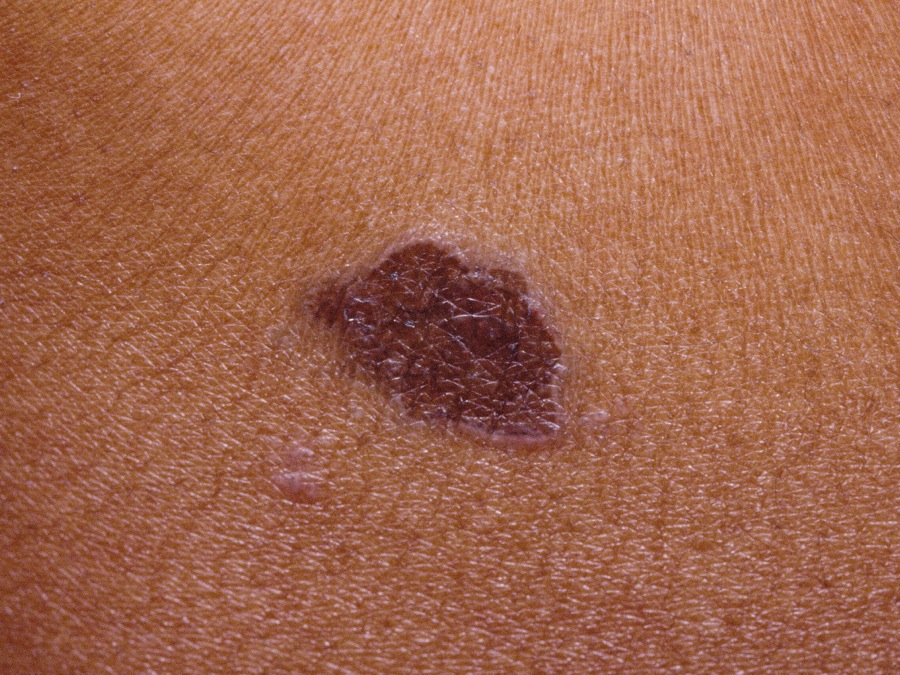
Post-inflammatory hyperpigmentation is common with LP>
Homepage | Who is Dr. White? | Privacy Policy | FAQs | Use of Images | Contact Dr. White