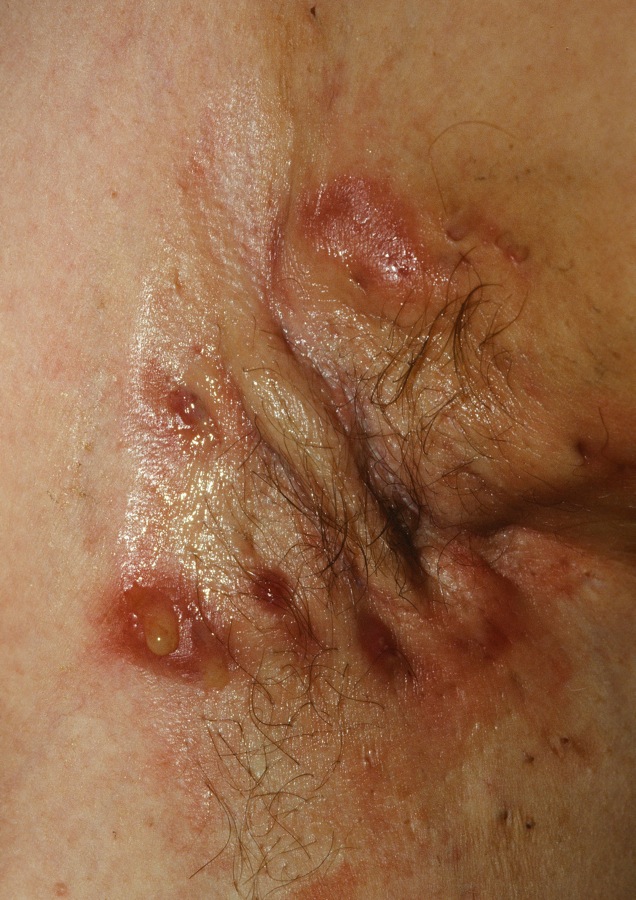
Multiple lesions with inflammation, drainage and scarring.

Multiple lesions with inflammation, drainage and scarring.
Hidradenitis suppurativa (HS) is a chronic inflammatory disease of the intertriginous skin areas, where hyperkeratinization of the epithelium causes pathologic hair follicle occlusion, with subsequent dilation and rupture. It is sometimes called “acne inversa,” although it is different from acne. HS is 2-4 times more common in females. It is also more common in African Americans. Onset is generally after puberty and most common between 20-24 years of age.
The lesions of HS usually start as a single inflamed, painful, raised nodule. The nodule either slowly disappears (between 10 and 30 days) or opens up, draining pus. Eventually, healing occurs but a scar may remain.
The patient is usually a woman with inflammatory nodules of the axilla and/or groin that may rupture, drain, and cause scarring. Some patients have more comedonal disease, others inflammatory nodules, and others erosive lesions. The perianal and inframammary areas are commonly affected as well. Sinuses, fistulas, and scars accumulate over time. Lesions are often quite painful or sore. Primary lesions are sterile but staphylococcal or other bacteria commonly infect secondarily. Rarely, a squamous cell carcinoma may develop in the setting of chronic HS. Chronic anemia may be associated and can cause chronic fatigu.
Patients with HS, and particularly women, experience great distress in their sex life. Embarrassment, frustration, and sadness are common. Asking a simple question about sexual satisfaction allows the patient, if she desires, to open up and express these feelings and may lead to better treatment approaches [JAAD Sept 2012].
Metabolic syndrome (MeS) combines obesity, dyslipidemia, hyperglycemia, and hypertension and is correlated with an increased risk for the development of cardiovascular disease. In one study of HS [JAAD April 2014], the prevalence of MeS was 50%.
Potential complications include keloid scars, fistulas, lymphedema, SCC, anemia of chronic disease, amyloid of the skin and/or kidney with the development of nephrotic syndrome, scarring, and limb contractures.
Patients with HS may develop systemic inflammatory response syndrome (SIRS) which is an exaggerated defense response of the body to a noxious stressor in an attempt to localize and then eliminate the endogenous or exogenous source of the insult. HS patients who present with sepsis-like features including tachycardia and leukocytosis should be considered for admission.
Cancer, in particular anogenital SCC may rarely occur [JAAD 2019;80;808]. The typical patient is one with long term, severe disease who develops a very painful nodule or lesion, often in the perianal or perineal area.
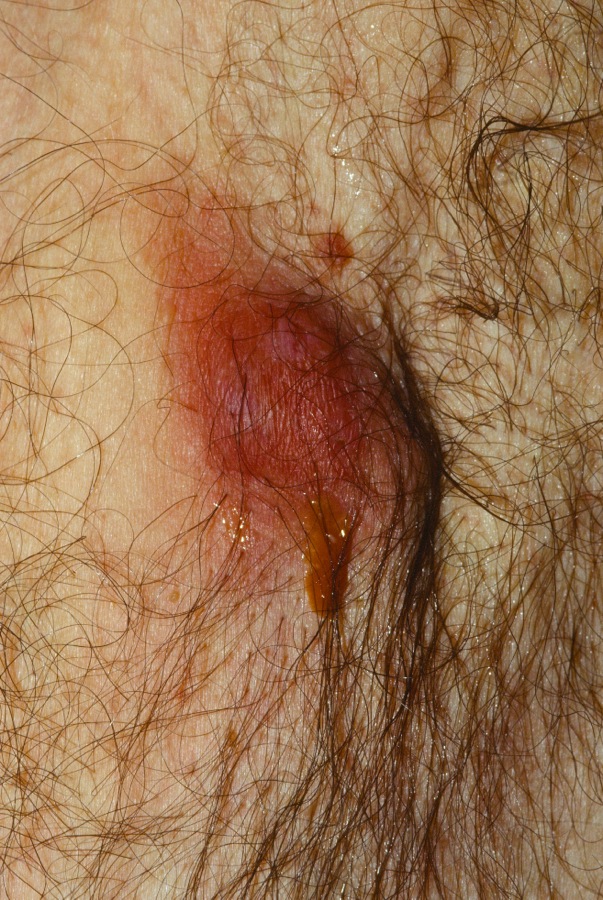
The bump may slowly resolve, or open up and drain as shown here.

Multiple lesions with inflammation, drainage and scarring.
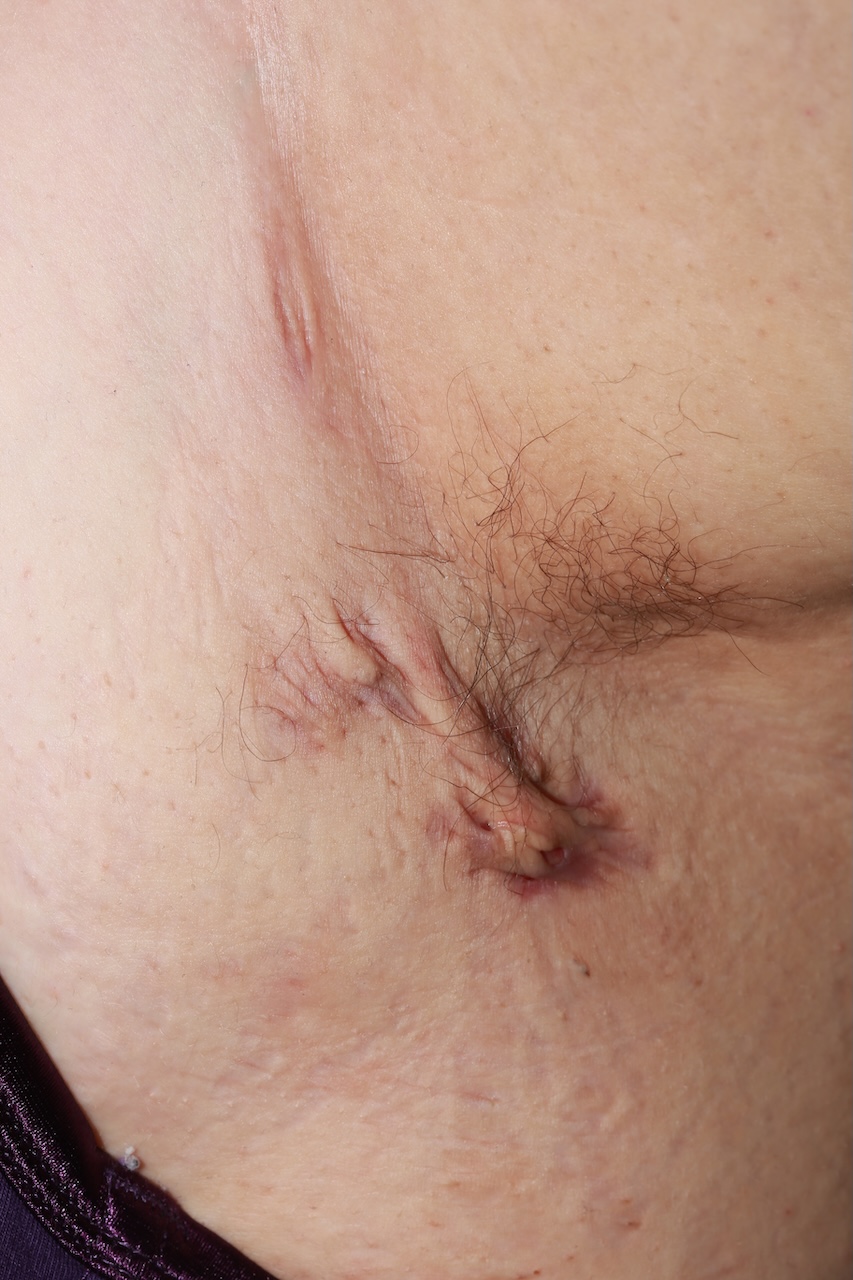 Once the inflammation has resolved, significant scarring may remain.
Once the inflammation has resolved, significant scarring may remain.
Who is Dr. White? | Privacy Policy | FAQs | Use of Images | Contact Dr. White